Your surgeon mentioned a procedure called EPP. They said it is the most aggressive surgical option for pleural mesothelioma. They said it removes the entire lung. You went home and tried to read about it on the internet. Half of what you found was confusing. The other half was terrifying.
This guide explains extrapleural pneumonectomy, almost always shortened to EPP, in plain language. You will learn what is removed, why some surgeons still recommend it, who is a candidate, what the risks really look like, and how it compares to the lung-sparing alternative P/D. The information here will help you ask better questions. The decision belongs to you and your surgical team.

What EPP Removes
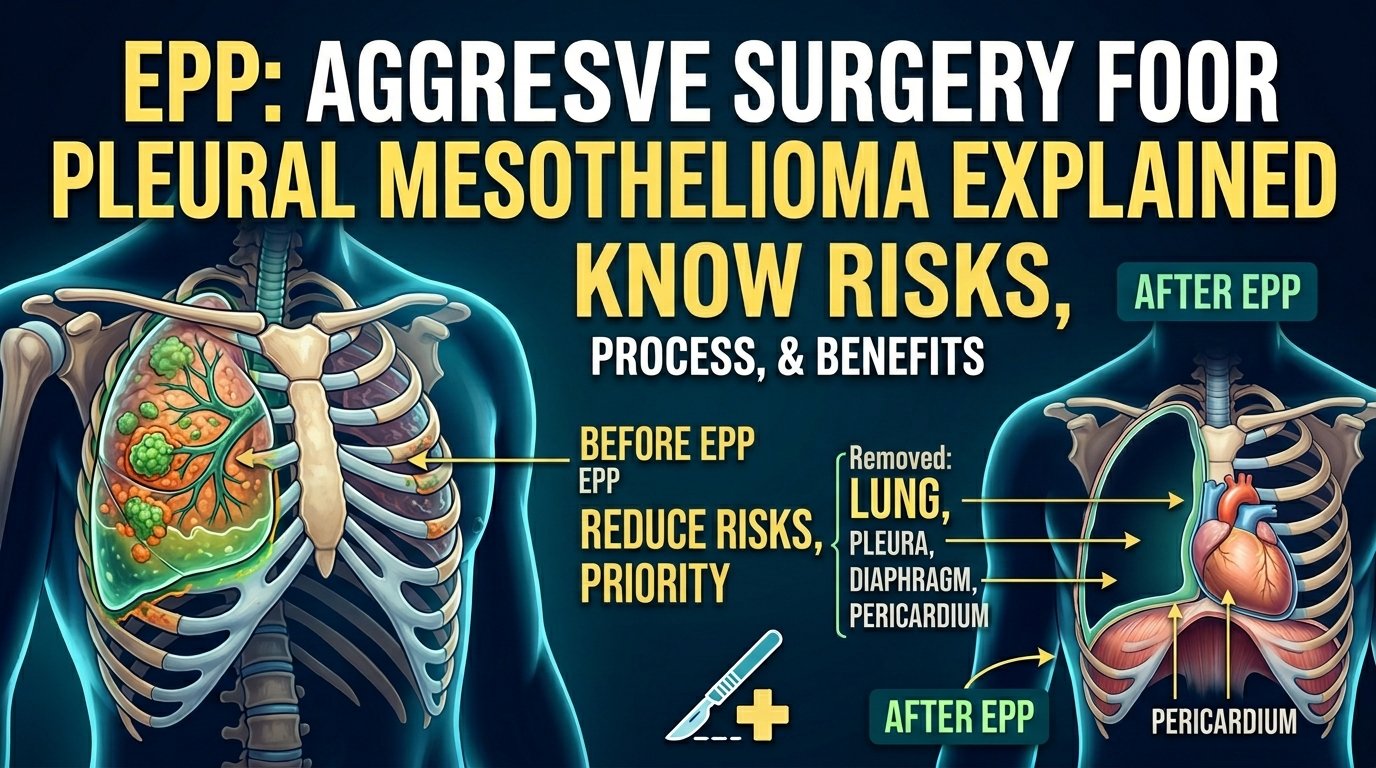
Extrapleural pneumonectomy is the surgical removal of an entire lung, the lining of the lung, the lining of the heart sac on that side, and a large portion of the diaphragm muscle. The diaphragm is then reconstructed with a synthetic patch. The pericardium, the heart’s lining, is also reconstructed if it was removed. This is a very large operation. It changes the anatomy of the chest permanently.
The reason surgeons developed EPP was the belief that mesothelioma cells are scattered throughout the chest cavity and the only way to achieve a complete cancer removal, what surgeons call macroscopic complete resection, is to take everything that could conceivably contain disease. The price is high. The patient lives the rest of their life with one lung and an altered chest cavity.
Why EPP Has Become Less Common
Twenty years ago EPP was the dominant operation for mesothelioma at the major centres. It is no longer. Most leading mesothelioma treatment centers now perform pleurectomy decortication, P/D, more often than EPP. The reason is data. Large studies have compared the two operations and found that P/D produces equivalent or better survival with significantly fewer surgical deaths and complications.
EPP carries an operative mortality rate of approximately five to ten percent at most centres, with some series reporting higher. Major complications occur in fifty percent or more of patients. The recovery is longer and harder than P/D. Pulmonary function is permanently reduced. Postoperative quality of life is meaningfully impaired.
For these reasons, the consensus has shifted. EPP still has a role, but it is reserved for specific cases where the tumour anatomy makes P/D impossible, or where a particular surgical team has consistently strong outcomes with EPP and the patient is fit enough for the operation. The choice is individual and should be made by an experienced thoracic team.

Who Is a Candidate Today
Modern EPP candidates are usually patients with epithelioid pleural mesothelioma, stage I or II disease, anatomy that makes lung-sparing P/D impossible or incomplete, intact pulmonary function on the contralateral side, intact cardiac function, no significant other medical conditions that would worsen surgical risk, and a clear understanding of what the operation entails.
Sarcomatoid mesothelioma cell type is generally considered a contraindication to EPP because the tumour biology is too aggressive for surgery alone to make a meaningful difference. Biphasic tumours occupy a middle ground and are evaluated case by case. Patients with significant heart disease, lung disease in the opposite lung, or poor functional status are usually not candidates.
The Operation in Detail
EPP takes six to ten hours in the operating room. The incision runs along the side of the chest. Once inside, the surgeon mobilises the lung, separates major blood vessels and the airway, and removes the lung along with the surrounding lining tissue in one large specimen. The diaphragm and pericardium are also removed and reconstructed.
Reconstruction uses synthetic mesh or patch material. The mesh diaphragm replacement allows the heart and other organs to remain in their normal positions and prevents abdominal contents from herniating into the chest cavity. The pericardial reconstruction prevents the heart from herniating, which is a rare but devastating complication if the pericardium is left open.
Blood loss during EPP is typically significant. Transfusions are commonly required. Anaesthesia is delivered through a special tube that selectively ventilates one lung at a time, allowing the surgical lung to be deflated for removal. The cardiopulmonary stress on the patient is substantial.
Recovery After EPP
The hospital stay after EPP is longer than P/D, often ten to twenty days. The first week is in a thoracic intensive care unit. Multiple chest tubes drain the empty cavity where the lung used to be. Fluid will fill that space slowly over weeks, eventually solidifying into scar tissue. The body adapts to having one lung over months. Pulmonary function tests at three months typically show roughly half the preoperative capacity, which improves slightly over the following year as the remaining lung compensates.
Daily life with one lung is possible but limited. Walking is fine for most patients. Stairs are slower. Vigorous exercise is constrained. Shortness of breath at exertion is permanent. The body learns to manage, but the experience is different from preoperative life.
Combining EPP With Other Treatments
EPP is rarely the only treatment. Most protocols combine EPP with chemotherapy before or after surgery, and sometimes hemithoracic radiation therapy after surgery to reduce local recurrence. The combination is called trimodality therapy. The radiation specifically targets the tissue that lined the empty cavity, attempting to kill any microscopic disease left behind.
This trimodality approach was the standard at major mesothelioma treatment centers for years. It is still used in select cases. The combined toxicity is significant, however, and many newer protocols favour P/D-based approaches that produce comparable outcomes with less morbidity.
Survival Outcomes
Median survival after EPP for selected epithelioid pleural mesothelioma patients ranges from eighteen to thirty-six months in most published series. Long-term survivors exist. Five-year survival in selected patient cohorts can reach twenty to thirty percent, though most series report lower figures. The variation reflects differences in patient selection, surgical experience, and adjuvant therapy choices across centres.
What the data has consistently shown is that the surgical team’s experience matters enormously. Outcomes at high-volume centres are dramatically better than at low-volume centres. If EPP is being recommended to you, ask the surgeon how many EPP operations they have performed personally in the last year. The answer should be in the double digits, not the single digits.
Questions to Ask the Surgical Team
If your team is considering EPP, ask the following questions explicitly. Why EPP rather than P/D in my case. What is your team’s operative mortality and major complication rate for EPP in the last year. What is your typical adjuvant therapy plan. What does my expected pulmonary function look like at three months and one year postoperatively. What is your protocol if the operation cannot be completed safely once you are inside the chest.
The answers will tell you a lot about whether this is the right team and the right operation. Surgeons who answer with specific numbers and clear rationale are usually the ones whose outcomes are the best. Surgeons who deflect or generalise should prompt you to seek a second opinion at another major mesothelioma treatment centers programme.
A Personal Decision
EPP is the most aggressive mesothelioma treatment option short of investigational therapies. For the right patient, it can produce meaningful long-term survival. For the wrong patient, it produces complications, reduced quality of life, and no benefit. The dividing line is patient selection, surgical experience, and clear-eyed expectations on the patient’s part.
If you are weighing EPP, get a second opinion at another high-volume centre. Ask both teams to explain their reasoning. The decision is permanent. Taking the time to be certain is worth it.
This article is for educational purposes and does not replace personalised guidance from a thoracic surgeon or oncologist. For evaluation, contact a high-volume mesothelioma treatment centre.